HPV vaccine lowers risk of Aids-related deaths
It is 7am in Nsanje District at the southern tip of Malawi and Eluby Albert, 45, has braved sweltering sunshine typical of the Shire Valley to receive HIV treatment.
The mother of five was found with the virus that causes Aids in April this year and this is her second visit to replenish the life-prolonging drugs at Nsanje District Hospital.
On this sunny morning, she is among a dozen men and women waiting to receive services that help people living with HIV stay healthy and live longer.
Albery cannot wait to get the drugs and return home to Suwali Village, Traditional Authority Malemia, along the banks of Shire River.
Every day, she buys fish from the country’s largest river for sale.
But that can wait.
During the meeting, she listened keenly as health workers took turns encouraging their clients to take antiretroviral (ARV) drugs without fail to boost their immune systems against opportunistic infections.
“Taking HIV treatment as prescribed will not only keep your immune system working and prevent illnesses but also suppress the viral load until the virus cannot be detected or transmitted,” says disease control surveillance assistant Susan Msiyambiri.
She also encouraged the clients to consider getting Covid-19 and HPV vaccines to increase their immunity. HPV causes cervical cancer, which accounts for 37 percent of new cancers in Malawian women, according to Doctors Without Borders.
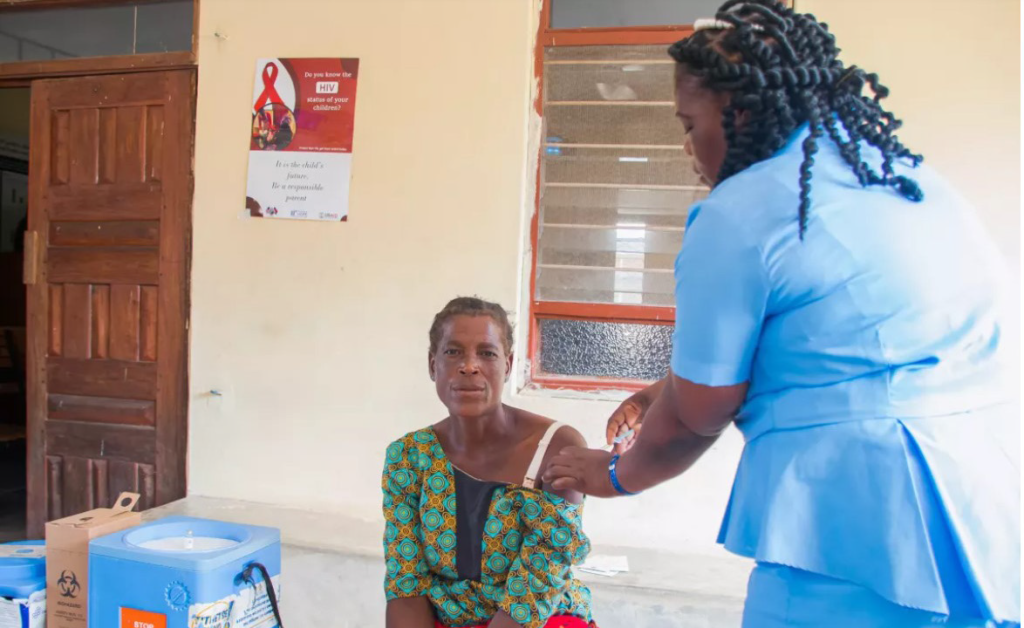
After the health talk, Albert was seen receiving the Covid-19 booster shot and HPV jab in a corner where Msiyambiri and another disease control and surveillance assistant Melody Chifudzeni were administering the vaccines.
The HPV vaccine was integrated in the HIV services to leverage resources and increase its uptake among adolescents living with HIV.
“These vaccines will help protect me from deadly diseases as HIV lowers immunity against various illnesses in the body. I have been sickly and often bedridden since last year. I was shocked but not surprised when I was found HIV-positive last month. I accepted the situation and vowed to do anything to protect my health,” Albert says.
The fishmonger envisions the vaccines, coupled with the ARVs, saving her life, business and dream of owning a decent house.
She feels lucky to get vaccinated against HPV.
Women with HIV are six times more likely to get cervical cancer, reports the World Health Organisation.
The Ministry of Health estimates that the silent killer claimed 2 905 lives from 4 145 confirmed patients in 2020, representing nearly eight deaths every day.
This is fuelled by delayed detection, scanty access to anti-cancer drugs, non-existent radiotherapy and a shortage of skilled hands to conduct life-saving surgeries.
“Prevention is better than cure. After all, we now get ART [antiretroviral therapy] services and vaccines under one roof, which saves time and money,” says Albert, whose husband died after a short illness in 2004.
Chifudzeni, who coordinates immunisation services at Nsanje District Hospital, says the vaccines are optional and clients receive adequate health tips to understand and distinguish the shots.
“After providing health tips, we only vaccinate interested clients. With Unicef support, we vaccinate 15 to 20 clients daily from Monday to Friday, which is good.
“Women with HIV undergo cervical cancer screening annually and a lot of our clients had cervical cancer too. So, it is essential to put HIV treatment and these vaccines in one safe space because they all target conditions that thrive on low body immunity,” said Chifudzeni.
Unicef, with financial assistance from Gavi, the Vaccine Alliance, supports the Ministry of Health in delivering Covid-19 and HPV vaccines alongside ART in 11 of the 15 health facilities in Nsanje District.
The initiative intends to increase Covid-19 vaccination among people living with HIV at the community and facility levels.
Nsanje district HIV and Aids coordinator McKnowledge Tembo says Unicef intervened after a year-long break in the integrated approach pioneered by Partners in Hope in 2022.
He said:“We vaccinated 2 000 people in 2022. Until Unicef intervened in April this year, we had no support to sustain the gains and safeguard our clients.
“The support for integrated services is essential because the risk factors of Aids, Covid-19 and HPV are the same. Low immunity and comorbidities put people with HIV at risk of dying from cervical cancer and Covid-19.”




